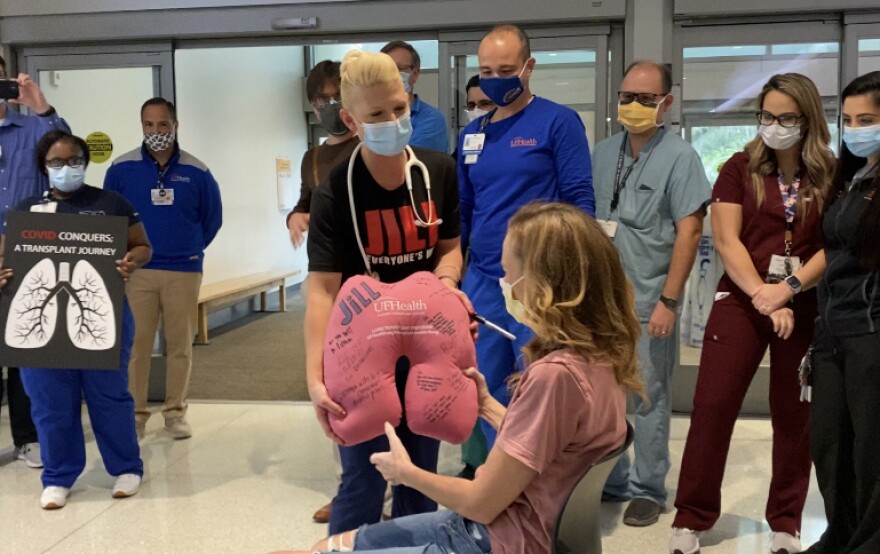
As a front-line intensive care nurse, Jill Holker cared for COVID-19 patients in Utah. When she contracted COVID-19 last fall, Holker suddenly became the patient fighting for her life.
Months of COVID-19 complications led to a double-lung transplant for Holker at the University of Florida Health Shands Hospital on Jan. 20. She was finally discharged Friday. Dozens of UF Health doctors, nurses and associates lined the halls of the UF Health Heart and Vascular Hospital to celebrate her release.
Before contracting the virus, Holker said she was healthy and active.
“Well I have no underlying health conditions at all,” she said. “I run, I work out, I work full-time, I don’t take any medications.”
Despite her health, COVID-19 severely struck Holker. UF Health doctors said she was unable to breathe on her own and had to be placed on extracorporeal membrane oxygenation, a life support treatment referred to as “ECMO.”
She was brought to Gainesville late last fall as doctors explored the possibility of a lung transplant. Andres Pelaez, lung transplant medical director at UF Health, said Holker was determined to be a strong candidate for the nine- to ten-hour surgery due to her previous health. He said she would not have been able to survive without the operation.
“Without the transplant she would not have been able to live,” Pelaez said. “She was that sick.”
UF Health Chief of Thoracic Surgery Tiago Machuca said lung transplants are complex procedures, especially in weakened COVID-19 patients.
UF Health’s lung transplant program was recently marked the best in the United States for one-year risk-adjusted survival rates, according to the Scientific Registry of Transplant Recipients. Throughout the past year, UF Health doctors said they have performed over ten double-lung transplants on COVID-19 patients. All have been successful.
Machuca said UF Health has been advancing in the volume and complexity of lung transplant operations performed over the past six years, priming the hospital to lead the way in treating COVID-19 patients through transplantations.
Machuca said it felt rewarding to perform these life-saving procedures.
“I think it gives us purpose,” he said. “So what is the purpose of our work? I think that’s it. It’s to see patients like Jill being able to walk out of here and get their lives back.”
Holker said she feels good and is grateful for her “second chance at life.” She also spoke to the importance of taking COVID-19 precautions, like wearing a mask, seriously.
“People need to just be safe,” she said. “Because this isn’t what I would wish on anybody. But I’m grateful that it was available.”
Holker said she will stay in Gainesville for about three months before heading back to Utah. As she continues her recovery, she said she plans to get back to running half-marathons next year.
Her doctors said they are confident she will reach this goal.
“I hope I can keep up with her,” Pelaez said.